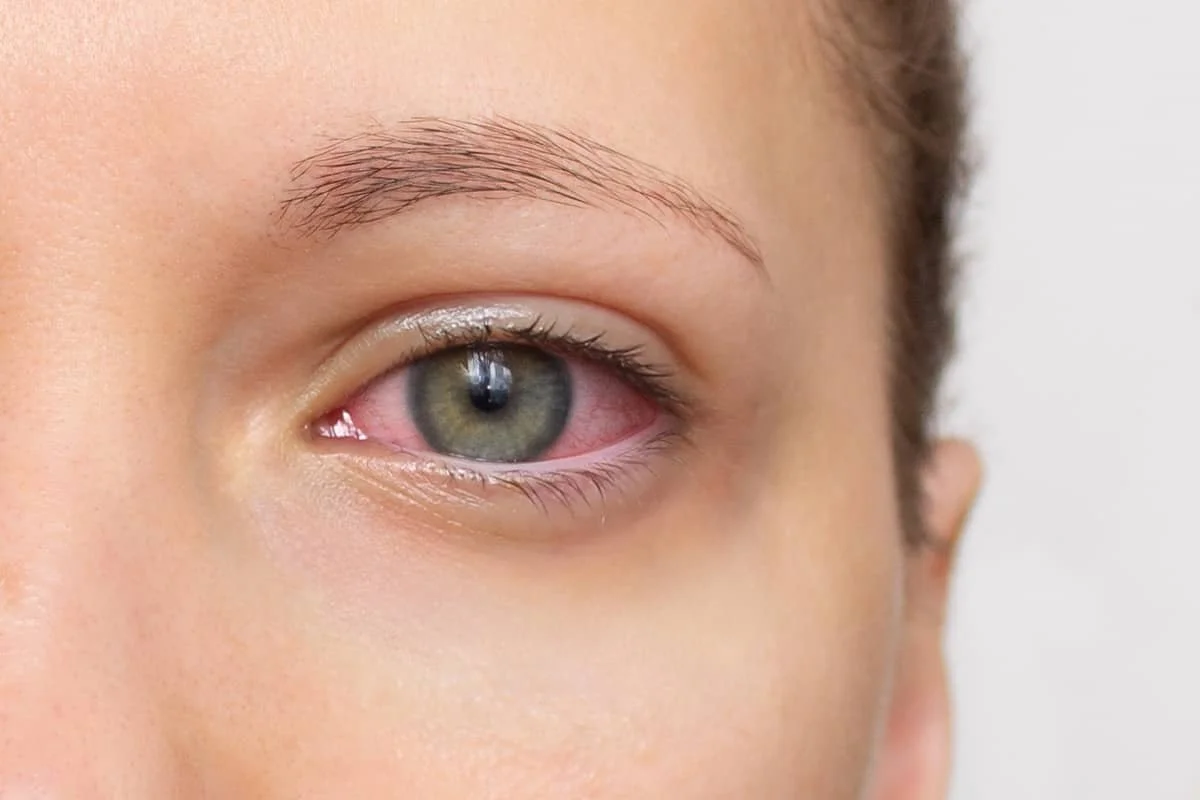
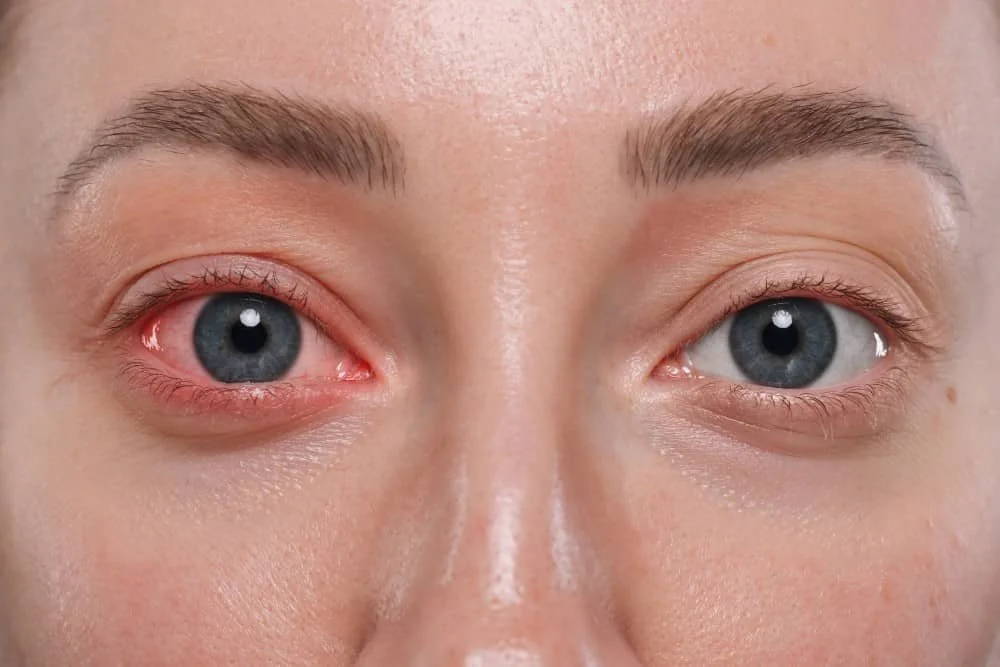
Red Eyes (Bloodshot Eyes): Why Are My Eyes Red and Should I Be Worried
Red or bloodshot eyes can be quite harmless, although there are some presentations that can be much more serious. Red eyes can have a variety of causes including irritants, injury, inflammation, and infection.
The following article lists a number of common red eye conditions, their associated symptoms, and recommended treatment.
What Are Bloodshot Eyes (Red Eyes)?
Some of the time both of your eyes may appear generally red following a late night or exposure to an environmental irritant (such as smoke). Bloodshot eyes occur when the tiny blood vessels on the eye’s surface expand.
Dilation of these vessels then causes their red colour to stand out in contrast to the whites of your eye. Redness can occur in one or both eyes, and can be localised to one area or cover the entire eye.
Symptoms
Symptoms of red eyes often include:
Redness or pinkness in one or both eyes
Grittiness, itchiness or a feeling of something being stuck in the eye
Watery eyes/excessive tearing
Photophobia (sensitivity to light)
Minor to severe pain
Blurry vision
Puffy eyelids
Causes of Red Eyes
Minor Causes of Red Eyes
Mild cases of red eyes should clear up within a few days without medical treatment. Simple lifestyle changes, such as hydration, rest, and avoiding any irritants is the best way to resolve any transient ocular surface irritation.
Causes of mild red eyes include:
Allergies
Sensitivity to environmental irritants, such as smoke, air pollution, chlorine, or perfume
Excessive screen time/digital eye strain [1]
Inappropriate use of contact lenses
Lack of sleep, alcohol consumption, drug use
Subconjunctival haemorrhage (burst blood vessel in one eye)
Conjunctivitis
Conjunctivitis, also known as pink eye, refers to inflammation at the lining of your eyelid and the white of your eye.
It most commonly occurs following exposure to bacteria, a virus, allergen, or other environmental irritant. [2] Symptoms generally include excess tearing, gritty/itchy/burning sensation, yellow discharge, and crusting of your eyelashes. [3]
This condition is particularly commonly among children and it is often very contagious. If you think you have conjunctivitis, avoid touching or rubbing your eyes and consider visiting our optometrists.
Subconjunctival haemorrhage
This condition occurs when one of the tiny blood vessels beneath the surface of your eye burst. This blood is then trapped and hence causes the white of your eye to turn bright red.
It can be caused by a strong sneeze, vomiting, or heavy lifting. Although this condition can look quite scary, it should be painless and will tend to self-resolve over days or weeks. [4]
If you’re taking blood thinners or the condition appears to be worsening, consider visiting our optometrists.
Blepharitis
Blepharitis is a condition involving inflammation of the lid margin and can be classified into 2 types, anterior and posterior.
Blepharitis can cause the eyes to appear red and will need to be managed appropriately, depending on the specific type. The following article goes into more detail about blepharitis, the various symptoms and corresponding management.
Learn more: What is Blepharitis? Symptoms, Risk Factor and Management
Dry eye
Dry eyes are caused either by the tears evaporating too quickly from the surface of your eye, or by the eyes not producing a large enough volume of tears.
Symptoms of dry eye may include excess tearing (as a reflex response to the surface dryness), sore/burning/gritty/irritated eyes, light sensitivity, and unstable vision between blinks. [5]
If you suspect you have dry eyes, it is important to consult our dry eye optometrists so that we can better determine the underlying cause of your condition and recommend treatment accordingly.
Eye injury
Eye injury or trauma can cause damage directly to the blood vessels in and around the eyeball.
Following an eye injury, you’re likely to experience pain, swelling, decreased vision, trouble moving the eyes in certain directions, and you may have a difference in pupil sizes.
Following an eye injury (or head trauma) it is important to seek professional advice urgently, or present to the emergency department at a public hospital, depending on the severity of your injury.
A less severe type of eye injury is a corneal abrasion. This occurs when a sharp object or other foreign material scratches the surface of your eye. [6]
Symptoms of this condition generally include excess tearing, pain, and decreased vision. Following a corneal abrasion, it is important to consult our optometrists so that we can determine the extent of your injury, and prescribe the appropriate treatment.
Inflammatory condition
Uveitis is a specific type of eye inflammation involving the middle layer of the eye (the uvea).
Symptoms of uveitis may include light sensitivity, haloes around lights, blurry vision, eye pain, changes to pupil size, and intense redness around the coloured part of your eye. [3]
If you notice these symptoms it is important to consult our optometrists promptly so that we can get the inflammation under control.
Chalazion and hordeolum
A chalazion or hordeolum are more commonly referred to as a ‘stye’ and tend to present on the eyelid as a red lump. [7] These may be uncomfortable but are generally painless, and are caused by a blockage in the oil gland. A warm compress (with a heat pack) and gentle massage can help disrupt this blockage, but if these lumps are chronic or recurrent, it is advisable to seek the opinion of our optometrists.
Acute closed-angle glaucoma
Acute closed-angle glaucoma occurs when there is a buildup of fluid in the front part of your eye. This fluid accumulation then causes severe pain in the affected eye, often accompanied by a headache, blurred vision, haloes around lights, and nausea/vomiting. [8]
If you suspect you’re suffering an acute closed-angle glaucoma attack it is essential to seek urgent medical advice. Our optometrists can identify this condition and act to start reducing the pressure inside your eye. Following this step, a referral to a hospital eye clinic or glaucoma specialist will be required for further preventative care.
Tips to help promote a healthy ocular surface to prevent bloodshot eyes
There are a variety of reasons why your eyes may be red, but the following tips are good for generally maintaining a healthy ocular surface.
Adequate hydration is especially important in the context of alcohol consumption (as alcohol causes dehydration and works to relax and dilate blood vessels within the eyes, in turn making them appear bloodshot)
It may be necessary to avoid having fans blowing overhead whilst asleep at night. This additional air movement can exacerbate underlying dry eye conditions. As an alternative, adding a humidifier to your environment can be hydrating to the eyes as it adds moisture to the air
Keep a bottle of non-preserved lubricating drops handy, so that you can instil these when you first notice your eyes becoming dry/gritty/irritated. These can be especially helpful if you spend extended periods of time at the computer
Avoid touching your eyes and face if your hands are not freshly washed, this way we can prevent the spread of infection, especially if you spend a lot of time with children
Remove eye make-up thoroughly at the end of each day. This will keep your eyelids and eyelashes clean and free from any build-up of excess debris or bacteria
Treatments for Bloodshot Eyes
Home treatments for red eyes may include:
Overthecounter non-preserved lubricating eye drops to help add moisture to the ocular surface and reduce irritation
Gently placing a cold compress over swollen eyelids (particularly if you have itchy, red eyes due to allergies)
Antihistamines or decongestants if your red eyes are from allergies
Wearing wraparound sunglasses in windy conditions or protective eyewear if exposed to irritants
Emergency red eye treatment may include
Steroid or antibiotic eye drops
Addressing eye injuries or untreated infections
Addressing underlying ocular conditions
Oral medication
When should you seek medical advice?
If you experience severe pain (or nausea/vomiting/fever) or you’re unable to open your eyes
If you have a foreign body in the eye or have suffered other eye trauma
If your vision has suddenly become blurry, or you suddenly notice haloes around lights
If you notice any thick mucous discharge
If you’ve recently had eye surgery (or an eye infection) and your vision is deteriorating
If your red eye(s) have lasted a number of days and are not improving [9]
Frequently Asked Questions
What does having red or bloodshot eyes mean?
Red eyes can indicate a wide range of issues, from minor irritation to serious health concerns. Red eyes usually indicate trauma to the eye, eye irritation, an eye condition, or a viral or bacterial infection.
Is a bloodshot eye something to be worried about?
Normally, red eyes are mild and temporary and not a cause for concern. However, severe or persistent red eyes may require medical evaluation.
What is the Difference Between Temporary and Chronic Bloodshot Eyes?
Most minor cases of bloodshot eyes heal within a few days. Some cases of red eyes can take a couple of weeks to heal.
If your red eyes still haven’t healed after two weeks, schedule an evaluation with our optometrists. When red eyes last for more than several weeks, it may be chronic red eyes or result of an underling health condition.
How do contact lenses contribute to red or bloodshot eyes?
Contact lens wear can cause red eyes if they are not properly maintained, overworn, or poorly fitted. Symptoms of CL over-wear can include irritated or watery eyes, swollen eyelids, general ocular surface redness, or eye pain more likely associated with an infection. [10]
Therefore, we strongly advise avoiding sleeping/showering/swimming in your lenses, and always handling your lenses with clean hands. Wearing contacts for too long at once, or overusing contact lenses over a long period of time can also compromise your eye health. If your eye becomes uncomfortable with contact lens wear please present to our optometrists in Fremantle.
When should you see a GP or an optometrist for red eye?
If ‘over the counter’ red eye treatments are not working (such as eye drops), you may need to see an optometrist or your GP. If red eyes last more than a week or two, consider booking a comprehensive eye exam to determine appropriate treatment.
References
[1]: Rosenfield, M. (2011) ‘Computer vision syndrome: A review of ocular causes and potential treatments’, Ophthalmic and Physiological Optics, 31(5), pp. 502–515. doi:10.1111/j.1475-1313.2011.00834.x.
[2]: Gin, C., Crock, C., & Wells, K. (2024). Conjunctivitis: A review. Australian Journal of General Practice, 53(11), 847–852. https://search.informit.org/doi/10.3316/informit.T2024111500010490530979611
[3]: Gupta, A., Bansal, R., Sharma, A., Kapil, A. (2023). Red Eyes—Conjunctivitis, Corneal Ulcers, Dry Eye Disease, and Acute Uveitis. In: Ophthalmic Signs in Practice of Medicine. Springer, Singapore. https://doi.org/10.1007/978-981-99-7923-3_17
[4]: Tarlan, B., & Kiratli, H. (2013). Subconjunctival hemorrhage: risk factors and potential indicators. Clinical Ophthalmology, 7, 1163–1170. https://doi.org/10.2147/OPTH.S35062
[5]: Bartlett, J. D., Keith, M. S., Sudharshan, L., & Snedecor, S. J. (2015). Associations between signs and symptoms of dry eye disease: a systematic review. Clinical Ophthalmology, 9, 1719–1730. https://doi.org/10.2147/OPTH.S89700
[6]: Wipperman JL, Dorsch JN. Evaluation and management of corneal abrasions. Am Fam Physician. 2013 Jan 15;87(2):114-20. PMID: 23317075.
[7]: Gordon, A.A., Danek, D.J. and Phelps, P.O. (2020) ‘Common inflammatory and infectious conditions of the eyelid’, Disease-a-Month, 66(10), p. 101042. doi:10.1016/j.disamonth.2020.101042.
[8]: Nüssle S, Reinhard T, Lübke J. Acute Closed-Angle Glaucoma-an Ophthalmological Emergency. Dtsch Arztebl Int. 2021 Nov 12;118(Forthcoming):771–80. doi: 10.3238/arztebl.m2021.0264. Epub ahead of print. PMID: 34551857; PMCID: PMC8841641.
[9]: Noble J, Lloyd JC. The red eye. CMAJ. 2011 Jan 11;183(1):81. doi: 10.1503/cmaj.090379. Epub 2010 Oct 4. PMID: 20921253; PMCID: PMC3017259.
[10]: Shahid, S.M., Ahmed, S.N. and Khan, Y. (2019) ‘Eye problems in contact lens wearers’, BMJ, p. l6337. doi:10.1136/bmj.l6337.